
Mental ill Health in a Parent or Carer
This procedure is to be used when considering the likelihood and severity of the impact of an adult's mental ill health on a child. It involves the practitioner using their professional judgement to balance the risk and protective factors for the child.
1. Introduction
1.1 Research indicates that 10–15% of children in the UK live with a parent who has a mental disorder.
1.2 A wide range of mental ill health can affect parents/carers of children and their families. This includes depression, anxiety and psychotic illnesses such as Schizophrenia or Bipolar Disorder.
1.3 Mental health issues can cause changes/difficulties with the way people think, feel or behave. Parental/carer mental ill health can, in some circumstances, lead to an inability to look after the child’s physical and emotional wellbeing. This is often for a short temporary period however for some individuals it can be more prolonged.
1.4 It is important to identify that:-
A mental illness is a clinically diagnosable disorder that interferes with an individual’s cognitive, emotional or social abilities. Diagnosis is generally made according to a classification system (ICD 10). It is estimated that mental illness will affect 1 in 4 of us at some time in our lives.
Mental health problems are typically less severe and of shorter duration than mental illness and may include mental ill health temporarily experienced as a reaction to life stressors.
1.5 Parental/carer mental illness does not necessarily have an adverse impact on a child’s development. Just as there is a range in severity of illness, so there is a range of potential impact on families. The consequent likelihood of harm being suffered by a child will range from a minimal effect to significant one. Research has shown that the adverse effects on children and young people are less likely when parental/carer mental disorders are mild, last only a short time, are not associated with family disharmony and do not result in the family breaking up. Where a parent/carer, has an enduring and / or severe mental illness children in the household are more at risk of, or experiencing significant harm.
1.6 Children may be protected from harm when the other parent/carer or a family member can respond to the child’s needs, and the child has the support of friends and other caring adults.
1.7 It is essential to assess the implications of parental/carer’s ill health for each child in the family. This would also include assessment of the impact on the family members of the social, physical ill health or substance use, difficulties that a parent/carer with mental illness may also be experiencing.
1.8 Offering treatment for mental ill health and appropriate additional support in addition to building resilience for families usually means that mental illness can be managed effectively and as a result parents/carers are able to care successfully for their children.
2. Young carers
2.1 Young carers are children who are caring for a parent, sibling or other relative/person. There is growing evidence pointing to the adverse impact on the health, future employment opportunities and social and leisure activities of those providing unpaid care, particularly in young carers. The 2011 Census indicated there are 181,000 children and young people under 18 in the UK providing some care to family, friends or neighbours.
2.2 Additional information around Young Carers can be found here: Specific Issues Affecting Young Carers
3. Common mental health conditions
3.1 Depression
- Feelings of hopelessness and worthlessness
- Poor motivation and deteriorating in functioning such as; avoiding daily tasks or neglecting self-care, loss of interest in activities that a person would normally enjoy
- Breakdown in relationships or avoiding contact with people leading to social isolation
- Feelings of exhaustion and poor sleeps patterns or sleep difficulties including oversleeping or not being able to sleep
- Poor self esteem
- Appetite changes such as overeating or reduced appetite
3.2 Anxiety
- Worrying – sometimes with unrealistic expectations or in regard to issues that may, on the face it, appear “trivial”
- Poor sleep patterns due to feeling overwhelmed with thoughts and anxiety
- Physical symptoms – e.g. feeling shaky or increased heart rate
- Sudden bursts of terror Physical symptoms e.g. feeling shaky, increased heart rate, chest pains, feeling faint
- Fears that may disrupt normally functioning e.g. fear of leaving the house or talk to people
- Phobia’s some common examples of phobia include; fear of spiders, dogs, insects, heights, enclosed spaces and flying
- Irrational thoughts or fixed beliefs about a certain fear, may experience fears of negative consequences e.g; fear of family member coming to harm if certain actions are not taken
3.3 Obsessive Compulsive Disorders
- Repetition of action or thought e.g. washing hands repeatedly or counting objects
- Intrusive thoughts that result in people developing compulsive behaviours to cope
- Ritualistic behaviours, e.g. Counting, tapping, touching objects or cleaning a certain amount of times or in a certain pattern/routine
3.4 Bipolar disorder
- Periods of elated mood resulting in behaviour changes and increased vulnerability associated with hypomania, including spending large amounts of money, inability to sleep or dis-inhibited behaviour Periods of depression
- Periods of elated mood where a person may present with psychotic symptoms associated with mania, such as someone believing they have special powers
- Periods of depression associated with symptoms listed above
3.5 Schizophrenia
- Inability to perform daily tasks
- Psychotic symptoms such as visual or auditory hallucinations, e.g. Seeing strange things or hearing voices Hearing voices
- Deterioration in functioning and withdrawal or isolation from social activities
- A person may appear distracted or confused during conversation, e.g. Having difficulty answering questions or following instructions
- Increased agitation or irritability
3.6 Personality Disorders
3.6.1 Personality Disorders are a type of mental health problem where your attitudes, beliefs and behaviours cause you longstanding problems in your life. Your experience of personality disorder is unique to you. However, you may often experience difficulties in how you think about yourself and others. You may find it difficult to change these unwanted patterns.
3.6.2 Symptoms can include:-
- Frequent mood swings,
- Impulsive behaviour,
- Self-esteem issues,
- Relationship difficulties
- Experiencing thoughts of self-harm or suicide.
3.6.3 A diagnosis of personality disorder can only be made by a mental health professional, such as a psychiatrist – not by a GP.
4. Parental mental ill health holds specific risks for children of particular age groups which include:
4.1 Babies up to 1 year old
- Inability of the parent to respond and nurture
- Lack of warmth
- Negative responses
- Poor attachment
- Inconsistency in parenting
4.2 Young children
- Behavioural problems
- Anxiety and withdrawal
- Conduct disorder
- Aggression towards family and/or peers anxiety and withdrawal
4.3 Adolescents
- Increased risk of developing a mental health problem
- Behavioural problems
- Conduct disorder
- Depression
- Difficulties at school
- Difficulty with friendships. (It should be noted that friends can act as confidants and offer support. However, in some circumstances the young person may find it difficult or embarrassing to consult with friends or may have limitations in leisure hours as they may have become responsible for practical tasks at home or emotional support of the parent or siblings).
If you have concerns regarding a client experiencing Mental Health concerns please consider the PAMIC tool below to support your decision making.
5. Tool for Assessing and Responding To The Impact of Parental Mental Ill Health on Children (PAMIC)
5.1 This practice tool is intended for use by anyone involved in:
- Providing services to adults who are parents and/or carers
- Providing services to children and young people
5.2 When to Use This Tool
5.2.1 This tool is to be used when considering how likely and with what severity an adults mental ill health will impact on a child. It involves the practitioner thinking about the nature of risk and also the protective factors for the child so it includes the practitioner’s professional judgement.
5.3 Process to follow
- Follow the flowchart below.
- Section 6: PAMIC Check (see below) will support your assessment.
- Section 7 (see below) will support you in decision making regarding consent, confidentiality and information sharing.
5.4 Record Keeping
5.4.1 The assessment and actions taken should be fully recorded along with the resulting outcomes on individual organisation recording systems.
6. 1 Assessing the Potential Impact of *Parental Mental Ill Health on Children
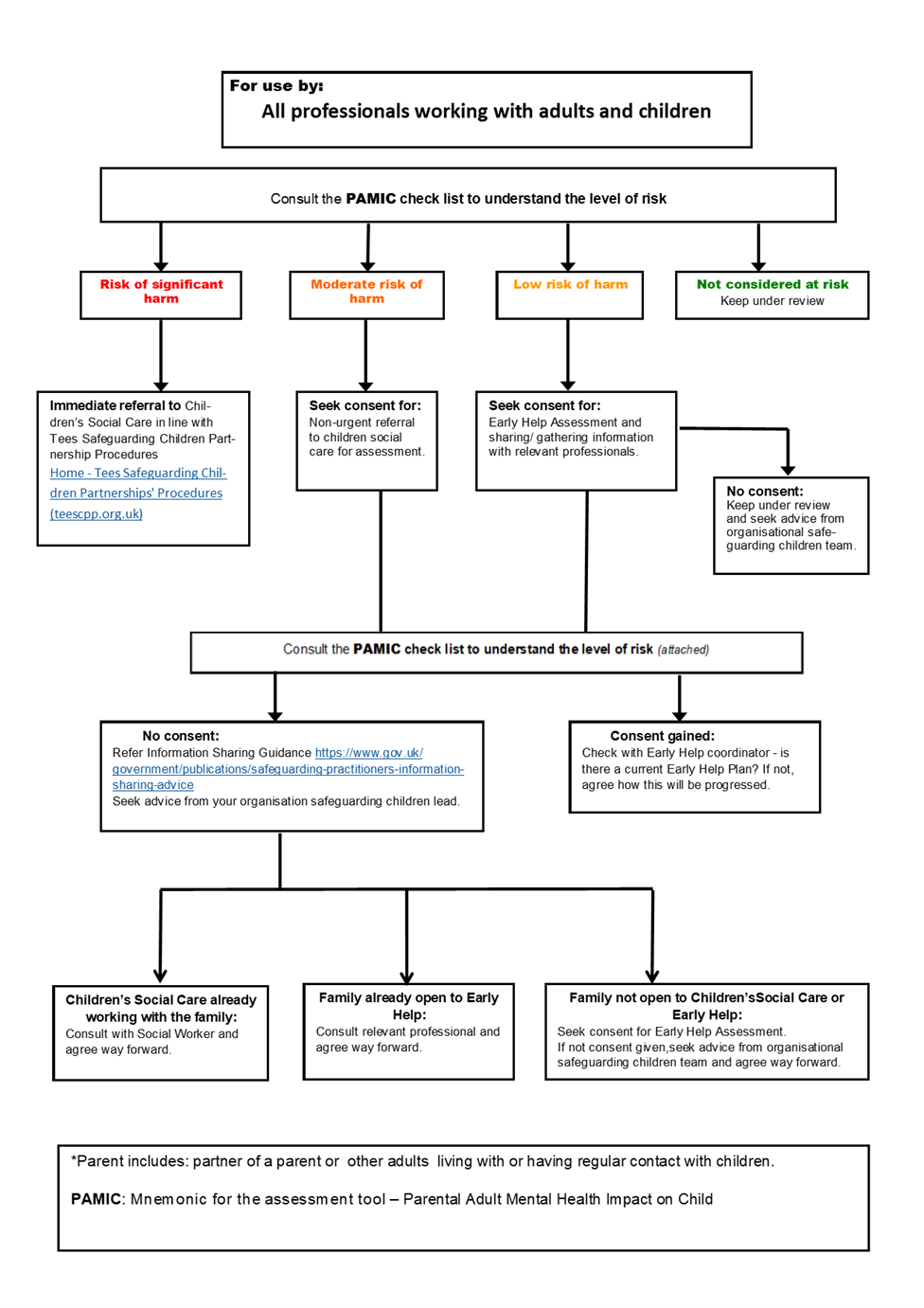
6. PAMIC Check - Potentiality for the Adult’s Mental Ill Health to Impact on the Child (updated June 2022)
The PAMIC check is a tool to support you when considering the likelihood and severity of the impact of an adult’s parental mental ill health on a child; it is not intended to replace professional judgement. You need to think about the nature of risk but also the protective factors for the child. When undertaking an assessment, consideration should always be given to any other current or previous safeguarding concerns particularly if those previous concerns have been associated with parental mental ill health. It is also important to understand if a family are open to Children’s Social Care or any other support services, including Early Help.
Examples of protective factors include:
- There is another adult that can be depended upon to meet the needs of the child and they are fully aware of the potential risk associated with parental/ carer mental ill health.
- The individual has insight into their problems, can take action to significantly reduce the impact of their behaviour on the child and is sufficiently supported.
Risk of Significant Harm - If any of the following factors are present they are highly likely to have a direct impact on the safety and well-being of the child. Immediate referral to Children’s Social Care in line with Tees Safeguarding Children Partnership Procedures Home - Tees Safeguarding Children Partnerships' Procedures (teescpp.org.uk)
- Delusional beliefs/ideas involving the child and or
- Risk that child will be harmed as part of a suicide plan.
- A pregnant woman has a history of post natal psychosis, particularly when this was associated with significant harm to a child.
- The child is a target for parental aggression or rejection.
- Co-existing domestic abuse, drug or alcohol abuse.
- There is no other adult that can be depended upon to meet the needs of the child. (Children of lone parents or isolated parents are at greater risk as they are less likely to have an alternative caregiver when a parent is in crisis).
- The child is the parent’s carer and this is impacting on the child’s welfare.
Moderate Risk of Harm - Where factors such as the following are present, although not of the same severity as above, they can potentially impact on parenting and result in concern for the child’s care. Seek consent for a referral to Children’s Social Care for an assessment.
- The presenting mental ill health (including the effect of medication/treatment) is impacting on the parents’ capability to consistently meet the needs of the child.
- The parental mental health disorder is designated ‘untreatable,’ either totally or within time-scales compatible with the child’s best interests.
- Where there is non engagement with mental health support services and it is considered that this could lead to potential risk to a child / unborn baby.
Low Risk of Harm - Where factors such as the following are present they require an assessment of the child’s needs to support planning for the child’s care. Seek consent for Early Help assessment.
- Parental learning disability rendering the child more vulnerable.
- Non-compliance or inconsistent compliance with treatment, reluctance or difficulty in engaging with necessary services, lack of insight into illness or its impact on the child.
- The child is vulnerable due to, for example, age, illness, disability or behavioural/emotional issues.
- Changes in the child’s behaviour since the onset of the parent/carer’s mental ill health.
Not considered at risk – No obvious impact on the child’s health and well-being are evident. Liaise with key others where appropriate and consent to do so is obtained. As events may change keep under review.
7. Confidentiality and Information Sharing
7.1 Information Sharing
Good information sharing is a crucial element of successful inter-agency working, allowing professionals to make informed decisions, thus improving outcomes for service users and children. Sharing of information is lawful where: ·
- The patient/client has consented for information to be shared.
- The public interest in safeguarding the child’s welfare overrides the need to keep information.
- Information must be shared under a court order or other legal obligation.
7.2 Information Sharing with Consent
7.2.1 Individuals can give their consent to personal information about them being shared with third parties, but it must be explained why this information is needed, what will be shared and who it will be shared with. If the information is sensitive in nature, for example relating to a person’s mental health, consent would need to be clearly recorded on the case file in line with organisational procedures.
7.2.2 A young person aged 16 years or over is capable to giving consent on their own behalf; children under 16 years can only give consent if it is thought that they fully understand the issues and are able to make an informed decision. If not, the decision must be made by the person who holds Parental Responsibility for them.
7.2.3 Where an adult is deemed incapable of giving consent to information sharing, consent should be sought, where possible, from a person who has the legal authority to act on that person’s behalf.
7.2.4 If it is not possible to obtain consent to information sharing, information can be disclosed without consent under the circumstances listed.
7.3 Information Sharing without Consent
7.3.1 Where consent has not been given, or it is thought that to seek consent from a parent or carer may place the child at further risk, professionals should consider whether it is lawful for them to share the information without consent.
7.3.2 Clearly, it would be lawful to share information in order to safeguard a child’s welfare, but professionals must consider the proportionality of disclosure against non-disclosure: is the duty of confidentiality overridden by the need to safeguard the child? Where information is shared, it should only be relevant information and only shared with those professionals who need to know. Professionals should consider the purpose of information sharing and remind those with whom information is shared that it is only to be used for that specified purpose and should otherwise remain confidential.
7.3.3 If practitioners are unsure whether it is appropriate to share information, they should seek guidance from organisational safeguarding/legal teams.
8. Further Guidance
Further guidance on information sharing with regard to safeguarding children is contained in Information Sharing (HM Gov; 2018) https://www.gov.uk/government/publications/safeguarding-practitioners-information-sharing-advice
and What to do if you are Worried a Child is being Abused (HM Gov; 2015) https://www.gov.uk/government/publications/what-to-do-if-youre-worried-a-child-is-being-abused--2
9. Useful Guidance Pathway Tools, Contacts and Websites:
9.1 Practice guidance produced by Social Care Institute for Excellence (2009) Think child, think parent, think family. London: SCIE